An Introduction to Decalcification

Decalcification describes the technique for removing minerals from bone or other calcified tissue so that good-quality paraffin sections can be prepared that will preserve all the essential microscopic elements. Decalcification is carried out after the specimen has been thoroughly fixed and prior to routine processing to paraffin. In this paper, the basic structure of bone is described and the technical options for preparing sections are outlined. The procedure for decalcification and the successful monitoring of the process is discussed and some popular options for the choice of reagents are provided.
Introduction
There are a number of options available when the histologist is required to produce sections from bone or other calcified specimens. In choosing a technique and processing method, consideration must be given to the type of investigation being carried out. For example, if a metabolic bone disease is being investigated and, it is necessary to differentiate mineralized bone from osteoid, or if morphometric measurements are required, it may be necessary to retain and demonstrate the mineral content by producing sections of undecalcified bone. As mineralized bone is such a hard material, there is a limited range of techniques available to produce sections from it. After fixation, it can be directly sawed into thin wafers and then ground using abrasive surfaces to produce thin “ground” sections (see Figure 1). It is also possible to prepare bone specimens by infiltrating them with acrylic or epoxy resins, which when polymerized, have a hardness equivalent to that of mineralized bone. You can then produce ground sections from the infiltrated specimens or section them directly using a heavy-duty microtome (such as the Leica SM2500) and a tungsten-carbide or diamond knife (see Figure 2). Frozen sections of mineralized cancellous bone are another possibility.1-3
Much more commonly, bone and other calcified specimens are decalcified (demineralised) following fixation and processed using a standard method to produce paraffin sections. Decalcified sections are used for the examination of bone marrow and for the diagnosis of tumours, infections, or for other purposes. The specimens may be in the form of iliac crest trephines, or bone pieces removed at operation (such as femoral heads) or dissected from amputation specimens. Fine detail radiographs are often used to assist in the selection of appropriate bone specimens for processing. Apart from bone, other tissues may undergo calcification associated with degenerative processes such as necrosis (dystrophic calcification), or it may occur in the walls of blood vessels or in kidney, lung, or elsewhere (metastatic calcification).4 If the calcified areas in tissue specimens are substantial, it may be impossible to obtain decent sections without first decalcifying the specimen. Another possibility is to apply “surface decalcification” to a paraffin block to allow sections to be obtained where the presence of calcium was not anticipated when the specimen was processed.
The decalcification procedure is relatively straightforward and is extensively discussed in standard texts of histological technique. 1-3 If high quality results are to be obtained however, some points are worthy of emphasis.
Structure of bone
Bone consists of cells (osteocytes) surrounded by a calcified matrix containing Type 1 collagen fibers. In the matrix, calcium is in the form of hydroxyapatite crystals [Ca10(PO4)6(OH)2] which are deposited between the fibrous elements. These crystals are dissolved out during the process of decalcification which, if performed correctly, leaves cohesive tissue with the physical characteristics of dense fibrous connective tissue.
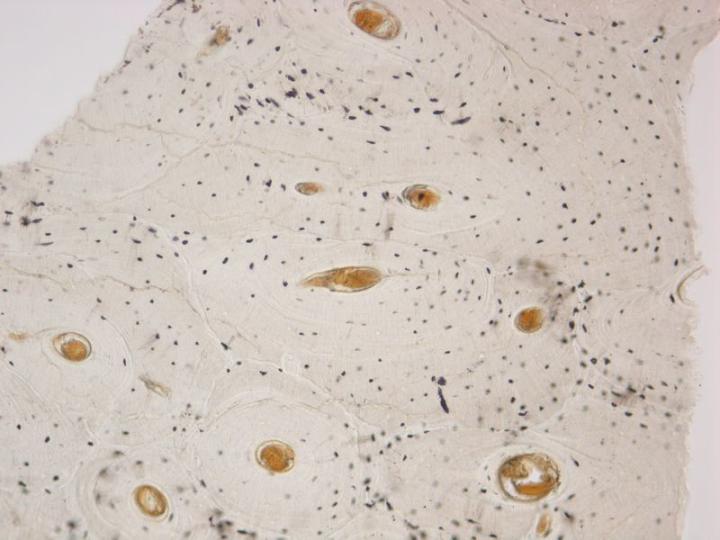
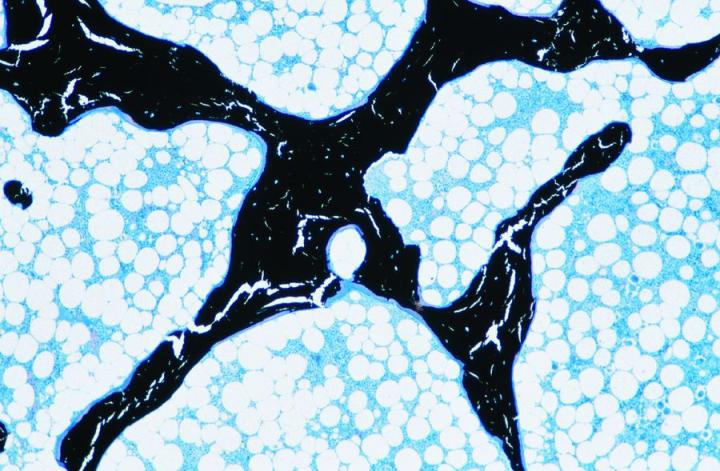
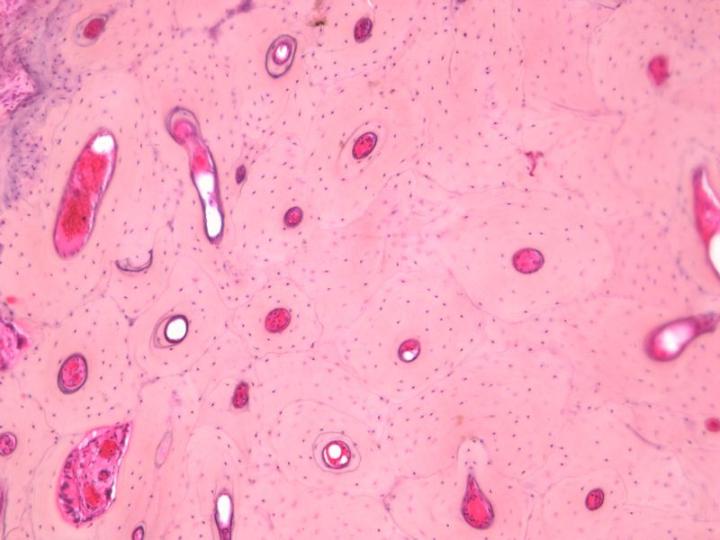
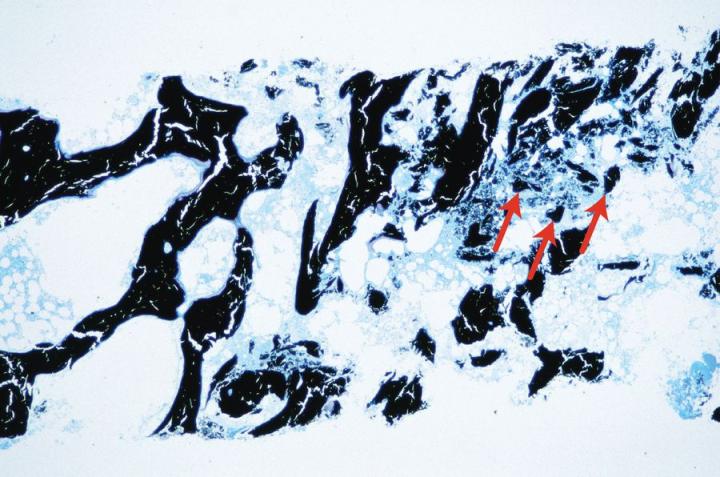
There are two types of mature bone. Cortical or compact bone forms the shafts of long bones and the major parts of the flat bones of the skull and has a very dense structure based on an arrangement of cylindrical structures called osteons (Figure 3). Cancellous, trabecular, or spongy bone has a much more delicate arrangement consisting of thin partitions (trabeculae) connecting bony plates between which is found the bone marrow. It is located in the vertebra and at the epiphyses of long bones (Figure 4). Both compact and cancellous bone develop in layers or lamellae in which the collagen fibers are structurally orientated and show a characteristic picture under polarized-light microscopy (see Figure 5).2-3, 5
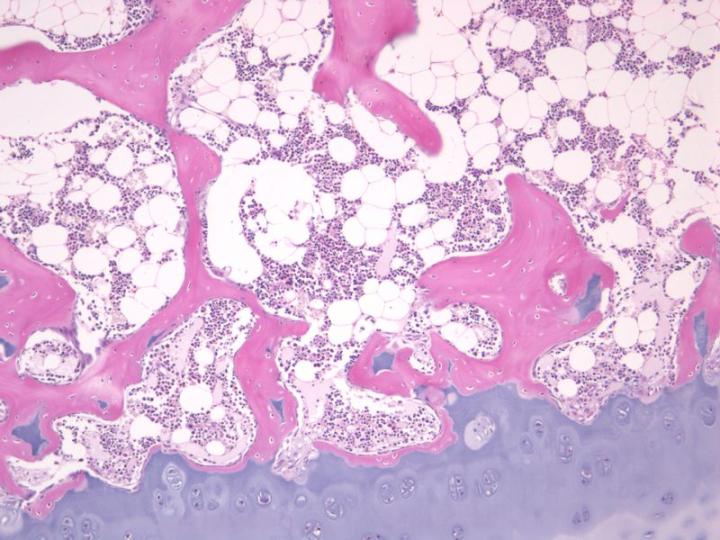

It is important to carefully consider the nature of any bone specimen received for processing because the relative amounts of cortical and cancellous bone are important and will determine the time required for decalcification and processing. For example, the iliac crest trephine specimen consists of a rim of cortical bone overlying a cylinder of cancellous bone. The cortical bone will be the last to give up its calcium salts during decalcification, and unless it is completely decalcified, difficulty will be experienced in obtaining decent sections.
Fixation of bone
In order to protect the cellular and fibrous elements of bone from damage caused by the acids used as decalcifying agents, it is particularly important to thoroughly fix these specimens prior to decalcification. 2-3 Poorly-fixed specimens become macerated during decalcification and stain poorly afterward. This is very noticeable in areas containing bone marrow. It is therefore common practice for laboratories to extend fixation times for bone specimens before commencing decalcification. It is important to provide ready access for the fixative to penetrate the bone, so skin and soft tissue should be removed from large specimens if practicable. Bone specimens should be sawn into thin slices as soon as possible to enhance fixation and an adequate volume of fixative provided. High-quality fine tooth saws should be used to prepare bone slices. Coarse saws can cause considerable mechanical damage and force bone fragments into the soft tissues present in the specimen (see Figure 6).
Buffered formalin is a satisfactory fixative for bone, but where the preservation of bone marrow is important, some laboratories will use alternatives such as one of the Zinc formalin mixtures, B5, formol acetic alcohol (Davidson’s fixative), or Bouin.
Decalcifying agents – Overview
There are three main types of decalcifying agents:
- Those based on strong mineral acids
- Those based on weaker organic acids
- Those composed of chelating agents.
For convenience, most laboratories choose from the many proprietary reagents available. Potential users of these products should consult the relevant MSDS to determine the active component present if it is not clearly stated in the technical information provided.
Decalcifying agents – Strong acids
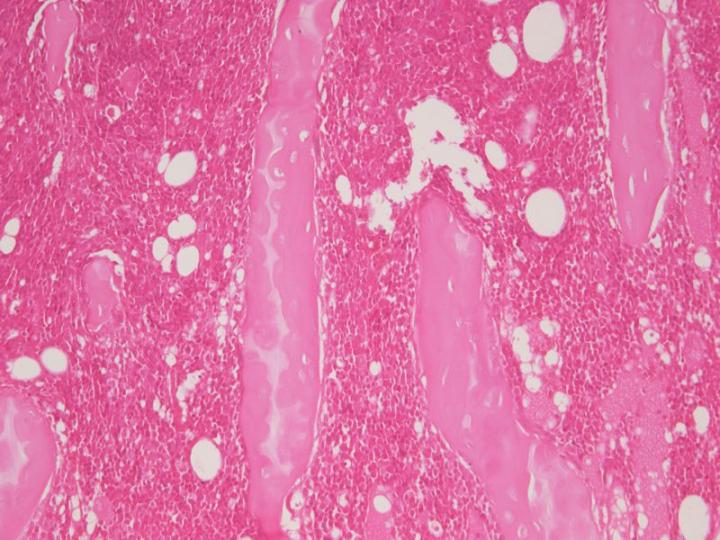
Strong acids such as hydrochloric or nitric acid at concentrations up to 10% are the most rapid in action, but if used for an excessive time, will rapidly cause a loss of nuclear staining and can macerate tissues. It is important that an appropriate end-point test is used to minimise exposure of the specimens to these agents. Generally, proprietary decalcifiers that are claimed to be rapid in action are based on strong acids, most commonly hydrochloric acid, and should be used conservatively with attention to the provided instructions if good results are to be obtained. For example, Surgipath’s Decalcifier II® is rapid in action and contains hydrochloric acid. Figure 7 demonstrates the consequences of prolonged treatment with a mineral acid decalcifier beyond the appropriate end-point.
Table 1 lists several of the more common mineral acid-based decalcifiers. Standard textbooks of histotechnology should be consulted for a more comprehensive listing.
Table 1: Mineral acid decalcifiers
|
Decalcifier |
Formula |
Comment |
|
Nitric acid6 |
5% in distilled water |
Rapid in action, exceeding end-point will impair staining. |
|
Perenyi’s fluid6 (1882) |
10% nitric acid 40ml 0.5% chromic acid 30ml Absolute alcohol 30ml |
A traditional decalcifier that decalcifies more slowly than aqueous nitric acid. Quite rapid in action, exceeding end-point will impair staining. |
|
Hydrochloric acid3 |
5-10% in distilled water |
Formalin should be washed from specimen before placing in HCl to avoid the formation of bis-chloromethyl ether (a carcinogen). Rapid in action, exceeding end-point will impair staining. |
|
Von Ebner’s solution6 |
Sodium chloride saturated soln. 50ml Distilled water 42ml Hydrochloric acid 8ml |
Rapid in action, exceeding end-point will impair staining. |
Decalcifying agents – Weak acids
Weak acids such as formic acid are popular and are widely used for decalcification. Formic acid can be used as a simple 10% aqueous solution or combined with formalin or with a buffer. Although it is slower than the strong acid agents, it is much gentler in action and less likely to interfere with nuclear staining. 1, 7 An example of a proprietary decalcifier based on formic acid is Surgipath’s Decalcifier I®. It also contains formalin and is claimed to fix as well as decalcify and be gentle in action. Other acids such as trichloracetic acid (TCA) have also been used. Picric acid, as a component of some fixatives, has weak decalcifying properties.
Table 2: Weak acid decalcifiers
|
Decalcifier |
Formula |
Comment |
|
Formic acid8 |
10% in distilled water |
A simple effective decalcifier. |
|
Evans and Krajian8 |
Formic acid 25ml Sodium citrate 10g Distilled water 75ml |
An effective formic acid decalcifier buffered with citrate. |
|
Kristensen8 |
Formic acid 18ml Sodium formate 3.5g Distilled water 82ml |
An effective formic acid decalcifier buffered with formate |
|
Gooding and Stewart8 |
Formic acid 5-25ml 40%formaldehyde 5ml Distilled water 75ml |
A formic acid decalcifier with added formalin, claimed to fix and decalcify. |
Decalcifying agents – Chelating agents
Chelating agents such as ethylenediaminetetracetic acid (EDTA) work by capturing the calcium ions from the surface of the apatite crystal, slowly reducing its size. Because the process is very slow but very gentle (weeks may be required depending on the size of the specimen), this reagent is not suitable for urgent specimens but more appropriate for research applications where very high quality morphology is required or particular molecular elements must be preserved for techniques such as IHC , FISH or PCR.9 It is used at a concentration of approximately 14% as a neutralized solution.1,10 The rate at which EDTA will decalcify is pH dependent. It is generally used at pH7.0. It works more rapidly at pH10, but some tissue elements can be damaged at alkaline pH. 10
Table 3: Chelating agents
|
Decalcifier |
Formula |
Comment |
|
Neutral EDTA1 |
EDTA disodium salt 250g Distilled water 1750ml Bring to pH 7.0 by adding sodium hydroxide (about 25g will be needed). |
Acts slowly but causes little tissue damage. Conventional stains are largely unaffected. |
Factors influencing the rate of decalcification
Concentration.
The concentration of active agent will affect the rate at which calcium is removed. Published formulations for decalcifying solutions strike a balance between speed and degree of tissue damage. It must be remembered that the concentration of active agent will be depleted as it combines with calcium and so it is wise to use a large volume of decalcifier and renew it several times during the decalcification process.
Temperature.
Increased temperature will speed up the decalcification rate but will also increase the rate of tissue damage so must be employed with great care.
Agitation.
Gentle agitation may increase the rate slightly.1
Fluid access.
As with fixation, fresh decalcifier should have ready access to all surfaces of the specimen. This will enhance diffusion and penetration into the specimen and facilitate solution, ionization, and removal of calcium.
Other techniques for increasing the efficiency of decalcification
Sonication used with EDTA has been successfully used to accelerate decalcification of trephine specimens for subsequent molecular analysis. During the process, the temperature must be carefully controlled.9 Microwave treatment has been used with hydrochloric acid decalcifiers, but the raised temperature may damage morphology and cause staining artifacts.10Ion-exchange resins have been incorporated into some decalcification protocols. They are added to the container holding the decalcifier and take up the ionized calcium maintaining the effectiveness of the acid. If acid decalcifiers are used in adequate volumes and replaced regularly, the use of such resins is probably unnecessary.3 Electrolytic decalcification in which the bone is placed in acid decalcifier and attached to an electrode through which current is applied is a technique that has not found wide acceptance because of the potential to cause heat damage to the specimen.3
Determining the end-point of decalcification
If high-quality results are to be obtained, it is important to determine the point at which all the calcium has been removed, because, from this point on, tissue damage seems to occur at an increasing rate. Over-decalcification, particularly with the strong acid decalcifiers, spoils the staining of basophilic elements such as cell nuclei and in some circumstances, can cause maceration of the softer tissue elements. On the other hand, specimens that are incompletely decalcified may be difficult or impossible to section.
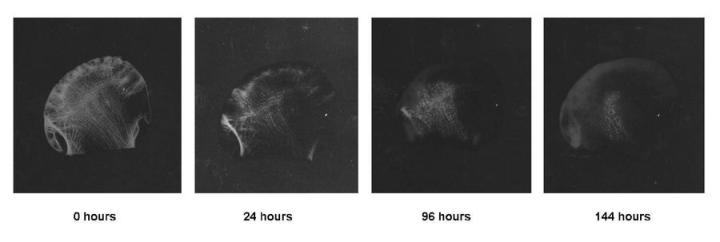
The best method, particularly with large specimens such as femoral heads, is to X-ray the specimen. A good-quality X-ray will clearly reveal tiny residual calcium deposits and allow further treatment if required. It is an excellent method for following the process of decalcification of large specimens such as femoral heads (see Figure 8). A simple chemical test can be applied when some acid decalcifiers are used (particularly formic acid). Ammonium oxalate solution is added to a sample of the final change of decalcified that has been neutralized with ammonium hydroxide.1If calcium is present, a precipitate of calcium oxalate will form indicating that decalcification is probably incomplete and a longer time in decalcified is required. Of course this test is best done on a relatively recent change of decalcifier (exposed to the tissue for say, one hour only). Physical tests require manipulation: bending, probing, or trimming of the specimen to “feel” for remaining calcified areas. Whilst this method may be successful in experienced hands, it is generally considered to be unreliable. Mechanical damage can occur during bending or probing, and small deposits of calcium can easily be missed.7 A method of determining the endpoint by carefully weighing the specimen after rinsing and blotting has also been described. This may be an effective method for large specimens.10
If you believe the decalcification end-point is close and you wish to slow the process down to avoid over-decalcification and consequent tissue damage, as might be the case when your laboratory is unoccupied during a weekend, specimens can be removed from decalcifier, rinsed, and placed back into formalin (important if hydrochloric acid is being used). Decalcification can then be resumed when convenient.10 An alternative is to refrigerate the specimen at 4˚C in its decalcifier to slow down the process.1

Treatment following decalcification and prior to processing
Various methods for neutralizing residual acid decalcifier before processing have been published, including extensive washing in tap water or the application of alkaline solutions. Generally a short, effective wash in tap water should be sufficient as any remaining acid will be removed during processing.1 It is important to remove the bulk of the decalcifier to avoid contaminating the processing reagents and the processor with acid.
Choosing a suitable schedule for decalcified bone or other decalcified tissues
Once the mineral has been removed a standard processing schedule can be used. It must be borne in mind that despite complete decalcification, bone, particularly compact bone, will contain dense areas that require thorough processing. It is better to use a schedule which is too long than too short. Your choice will depend on the nature and size of the specimen. Application of vacuum during wax infiltration should improve the quality of the finished blocks.
Surface decalcification
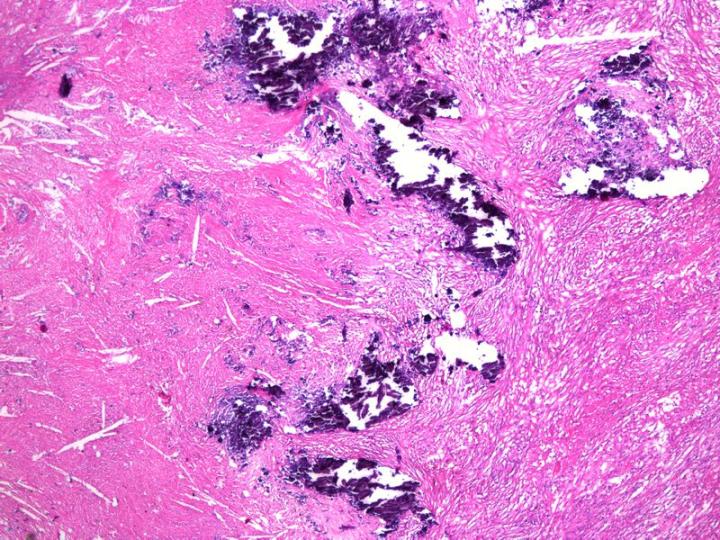
This is a method of dealing with small unexpected deposits of calcium that may be encountered in paraffin blocks (see Figure 10). Normally it is after trimming the block in the microtome to expose the specimen that the calcium is discovered. It is important at this stage to try to avoid disrupting the block surface extensively. After the tissue has been exposed, the block can be removed from the microtome and placed face down in an acid decalcifier for 15 – 60 minutes. This surface treatment will allow the decalcifier to penetrate a small distance into the block and dissolve the calcium. The block can then be thoroughly rinsed in water to remove residual acid, chilled, and sectioned. Careful realignment of the block will be required because the decalcifier will penetrate a very small distance into the block allowing only a couple of sections to be taken.1, 11
Conclusion
Decalcification is a straightforward process but to be successful requires:
- A careful preliminary assessment of the specimen
- Thorough fixation
- Preparation of slices of reasonable thickness for fixation and processing
- The choice of a suitable decalcifier with adequate volume, changed regularly
- A careful determination of the endpoint
- Thorough processing using a suitable schedule.
About the presenter

Geoffrey Rolls is a Histology Consultant with decades of experience in the field. He is a former Senior Lecturer in histopathology in the Department of Laboratory Medicine, RMIT University in Melbourne, Australia.
References
- Page KM. Bone. In Bancroft JD and Stevens A eds. Theory and Practice of Histological Techniques. New York: Churchill Livingstone, 1996.
- Moore RJ. Bone. In Woods AE and Ellis RC eds. Laboratory histopathology. New York: Churchill Livingstone, 1994;7.2-10.
- Carson FL. Histotechnology. 2nd ed. Chicago: ASCP Press, 2007.
- Vardaxis NJ. Pathology for the health sciences. Melbourne: Macmillan Australia Pty Ltd, 1997.
- Young B, Heath JW. Wheater's Functional Histology. 4th ed. Edinburgh: Churchill Livingstone, 2000.
- Clayden EC. Practical section cutting and staining. Edinburgh: Churchill Livingstone, 1971.
- Skinner RA, Hickmon SG, Lumpkin CK, Aronson J, Nicholas RW. Decalcified Bone: Twenty Years of Successful Specimen Management. The Journal of Histotechnology 1997;20;267-277.
- Wallington EA. Histological Methods for Bone. London: Butterworths, 1972.
- Reineke T, Jenni B, Abdou MT et al. Ultrasonic Decalcification Offers New Perspectives for Rapid FISH , DNA, and RT_PCR Analysis in Bone Marrow Trephines Am J Surgical Pathology 2006;30.
- Callis G, Sterchi D. Decalcification of Bone: Literature Review and Practical Study of Various Decalcifying Agents, Methods, and Their Effects on Bone Histology. The Journal of Histotechnology 1998;21;49-58.
- Rolls GO. Difficult Blocks and Reprocessing. Leica Microsystems, 2011.
Related Content
Leica Biosystems Knowledge Pathway content is subject to the Leica Biosystems website terms of use, available at: Legal Notice. The content, including webinars, training presentations and related materials is intended to provide general information regarding particular subjects of interest to health care professionals and is not intended to be, and should not be construed as, medical, regulatory or legal advice. The views and opinions expressed in any third-party content reflect the personal views and opinions of the speaker(s)/author(s) and do not necessarily represent or reflect the views or opinions of Leica Biosystems, its employees or agents. Any links contained in the content which provides access to third party resources or content is provided for convenience only.
For the use of any product, the applicable product documentation, including information guides, inserts and operation manuals should be consulted.
Copyright © 2025 Leica Biosystems division of Leica Microsystems, Inc. and its Leica Biosystems affiliates. All rights reserved. LEICA and the Leica Logo are registered trademarks of Leica Microsystems IR GmbH.