
Overview of Biopsy Procedures and Experiential Data Analysis from a Comprehensive US Hospital Network Breast Center

A biopsy guides diagnosis, the need for further testing, disease progression and treatment. In this article different types of biopsies are defined, as well as who performs the biopsy and what happens once the biopsy leaves the body.
A biopsy is the removal of cells or tissue from the body to be examined in a laboratory by a pathologist to determine abnormalities (such as those caused by inflammatory and autoimmune disorders or infection) or diseases such as cancer. Biopsies are also used to match organ tissue before a transplant and to look for signs of organ rejection following a transplant.
Almost any organ in the body can be biopsied as well as the bones, bone marrow, thyroid, lymph nodes, muscles and nerves.1 Biopsies can be excisional where a whole lump or targeted area is surgically removed, or incisional/core biopsy where just a tissue sample is taken. 2
Types of Biopsies
The different types of biopsies include the following:3
- Shave biopsy – a piece of skin is removed or scraped using a sharp blade. A shave biopsy is only used for growths or abnormal areas that are on the top or outer layers of skin. This includes the epidermis and the outermost part of the dermis. A shave biopsy is mainly performed to diagnose types of non-melanoma skin cancer such as basal cell carcinoma and squamous cell carcinoma. It is also used to diagnose other skin tumors including actinic keratosis (a precancerous condition of the skin) and non-cancerous skin tumors or conditions such as seborrheic keratoses.4 Since a shave biopsy is superficial, it does not require stitches. A scab will form and will usually heal in 1-3 weeks. The drawback of this procedure is that a pathologist may have difficulty identifying or ruling out invasive disease.
- Punch biopsy – a circular blade is used to obtain full thickness skin specimens. The instrument goes through the epidermis and dermis into the subcutaneous fat.5 A punch biopsy is used to diagnose precancerous skin conditions, non-cancerous skin tumors or conditions as well as many types of cancers including non-melanoma and melanoma skin, mouth (oral cavity), throat (oropharyngeal and hypopharyngeal), inflammatory breast, vaginal, and vulvar. After the punch biopsy procedure, 1-2 sutures may be required to close the wound and control bleeding.6
- Needle biopsy – a needle is used to take tissue or fluid samples from muscles, bones, and other organs, such as the liver or lungs. There are several types of needles that may be used. A fine needle biopsy uses a needle smaller than a venipuncture needle that is attached to a syringe. A core needle biopsy is an inner needle connected to a trough, covered by a sheath, and attached to a spring-loaded device. A vacuum assisted biopsy uses a vacuum to obtain larger pieces of tissue. Needle biopsies are performed with guidance such as MRI, ultrasound, CT (computed tomography), or fluoroscopy. A local anesthetic is administered.
- Bone Marrow aspiration and biopsy – is used to determine blood disorders or blood cancer such as leukemia, lymphoma, or multiple myeloma. The biopsy is performed by inserting a small needle into the bone and removing bone marrow tissue.
- Capsule biopsy – The capsule biopsy is used to obtain non-endoscopic intestinal biopsy specimens.
- Esophagogastroduodenoscopy (EGD) biopsy – An EGD is a procedure used to examine the lining of the esophagus (swallowing tube), stomach, and upper part of the small intestine (duodenum). When needed, an EGD is the current standard for obtaining biopsies from the upper gastrointestinal tract.7 It requires conscious sedation or general anesthesia.
- Colposcopic biopsy – A colposcope (a close focusing telescope with a bright light) is used to examine the cervix, vulva, and vagina. A cervical or vaginal biopsy could be performed during colposcopy and may require a local anesthetic.
- Cone biopsy – is performed to remove cervical tissue using three different techniques: 1.) a thin wire loop heated by electricity - Loop electrosurgical excision procedure (LEEP) 2.) a scalpel – Cold Knife Excision or 3.) a laser – Laser Excision. The cone biopsy may be completed using a local or general anesthetic in an outpatient setting.
- Laparoscopic biopsy – is a biopsy used for the abdomen that is performed by inserting a thin tube with a video camera called a laparoscope into the abdomen through a small incision to take a tissue sample.
- Stereotactic biopsy of the breast – uses mammography to target and locate an area of concern from two different angles of the same location of the breast using a hollow needle to obtain a biopsy. This is done using local anesthetic.
- Stereotactic biopsy of the brain – under general anesthesia in the operating room using a MRI or CT imaging study, a neurosurgeon takes a small piece of tissue from the brain, scalp, blood vessels, or dura mater using a stereotactic biopsy needle.8
- Liquid biopsy – also known as circulating tumor cell count or circulating tumor, DNA is a test performed on a sample of blood to look for cancer cells or pieces of DNA from tumor cells. The test may help determine early stages of cancer, treatment planning, how well the treatment is working, or if the cancer has reoccurred.9 Currently, the medical applications of liquid biopsies are limited to determining prognosis in breast, colon, and prostate cancer, guiding treatment in those cancers, and guiding treatment of non-small cell lung cancer.10
Depending upon the type of biopsy needed, the procedure may be performed by a surgeon, oncologist, gastroenterologist, radiologist, dermatologist, gynecologist, or family practice physician. Also, the type of anesthesia (local anesthesia, conscious sedation, or general anesthesia) the patient receives is determined by the type of biopsy performed. Biopsies are generally minimally invasive and safe. Complications that may occur as a result of a biopsy include:
- Bleeding
- Infection
- Accidental injury to adjacent structures such as the bowel during abdominal biopsy or lung parenchyma during renal biopsy11
After the biopsy specimen has been collected, it is placed into a container with fixative and delivered to a pathology laboratory. Once it arrives in the laboratory, the sample is examined by a pathologist or trained assistant. For relatively small sample biopsies, the entire tissue is put through several processes which results in the tissue being placed into a paraffin wax block. That paraffin block is sliced into ultra-thin sections which are then placed onto glass slides. The slides are then stained with dyes to highlight different cell structures viewable under a microscope.12 A pathologist examines and analyzes the slides and creates a report. The pathology report describes the organ or tissue biopsied, the specific part of the organ or body where the sample came from, the biopsy procedure, specific findings in the tissue, and other important results. The pathologist will give a final diagnosis, comment on areas of concern, and may recommend further testing. If the diagnosis remains uncertain after a technically successful procedure, a re-biopsy or a surgical biopsy may be necessary.
Biopsy results are usually available within 2-3 days. If more extensive or complicated testing needs to be completed, it may take 7 – 10 days.13 To further classify the tumor or determine treatment planning, molecular or genetic testing may be completed along with or after diagnosis.
Biopsy Procedure Observations
The following is an example of biopsy procedures observed by the Leica Biosystems Content and Evidence team during an on-site engagement at a nonprofit comprehensive hospital network breast center. The primary objective of this engagement was to observe the activities within the hospital to provide the data and metrics necessary to drive quality improvements and improved efficiencies for breast center patients.
Methodology
Four ultrasound breast biopsy processes were observed. A spring-loaded core needle device was used for all breast biopsy procedures.
Workflow Steps were as follows:
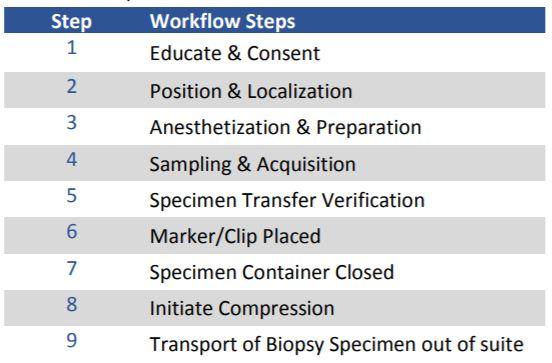

Results
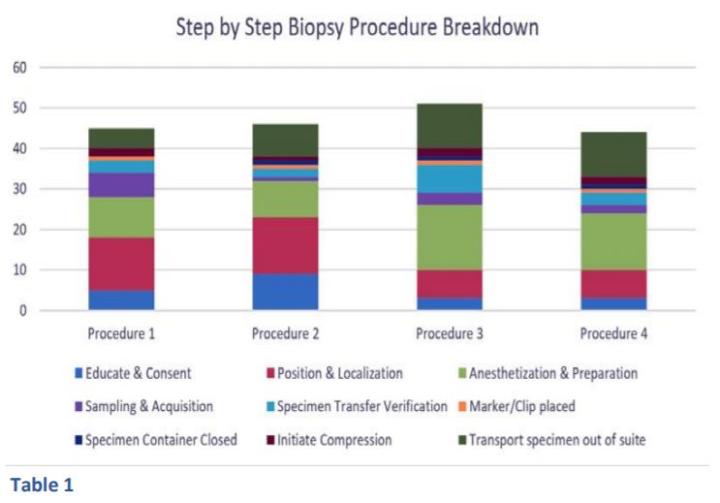
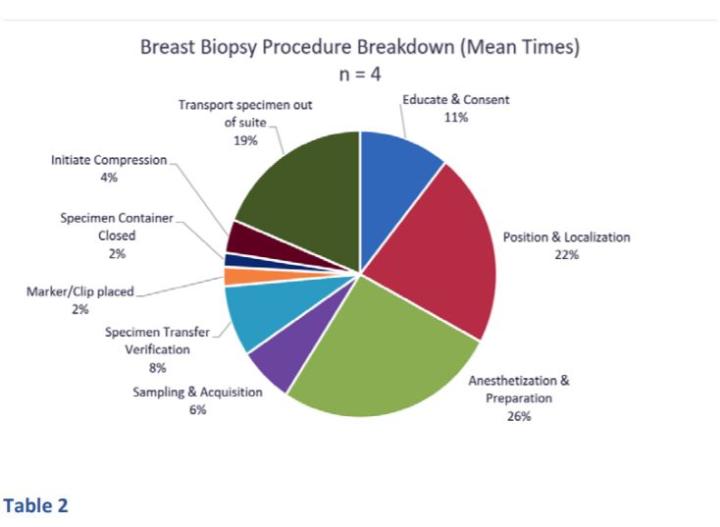
The step by step biopsy procedure breakdown (Table 1) and the mean times for all biopsies (Table 2) are displayed below. Procedure time for all procedures ranged from 44 minutes to 51 minutes. This time did not include room prep or transport of the biopsy specimen to the pathology lab. The longest step in the procedure was anesthetization and preparation (26% of procedure time or 12.25 minutes) while the sampling and acquisition represented only 6% or 3 minutes of the entire mean procedure time.
Conclusion
Based on our observations, biopsies performed for the diagnosis of breast cancers show that anesthetization and preparation are the steps that require the greatest time intervals. Prior to our observations, we expected much of the time to be spent on sampling and acquisition.
A biopsy is the most accurate way to determine what is going on in the body. It defines whether the abnormality is cancer or some other medical condition of concern. The biopsy guides diagnosis, the need for further testing, disease progression and treatment. Up to 70-80% of decisions affecting diagnosis or treatment involve pathology.14 Therefore, the laboratory and pathologist play key roles in the biopsy analysis process that ultimately determines a patient’s treatment plan, prognosis, and even outcome.
About the presenter

Rhondalyn Bomkamp, is an accomplished Director/Nurse Leader with a proven track record of effectively managing complex projects and health system performance improvement initiatives. As a registered nurse, she has experience in Quality and Patient Safety and Project Management/Development in the oncology, cardiac and intensive care arenas. She has strong clinical knowledge and management experience with the ability to recognize opportunities for improvement, coordinate the work of many areas and develop collaborative relationships with diverse groups to facilitate the implementation of change.
References
1.Biopsy Overview; RadiologyInfo.org; https://www.radiologyinfo.org/en/info.cfm?pg=BiopGen
2. Biopsy: What you need to know; Medical News Today; https://www.medicalnewstoday.com/articles/174043; March 2017
3. Cancer.Net https://www.cancer.net/navigating-cancer-care/diagnosing-cancer/tests-and-procedures/biopsy
4. Shave Biopsy; Canadian Cancer Society; https://www.cancer.ca/en/cancer-information/diagnosis-and-treatment/tests-and-procedures/shave-biopsy/?region=qcc
5. Zuber, Thomas J., M.D., Saginaw Cooperative Hospital, Saginaw, Michigan; Punch Biopsy of the Skin; American Family Physician; 2002 Mar 15;65(6):1155-1158.; https://www.aafp.org/afp/2002/0315/p1155.html
6. Punch Biopsy; Canadian Cancer Society; https://www.cancer.ca/en/cancer-information/diagnosis-and-treatment/tests-and-procedures/punch-biopsy/?region=on n
7. Otuya, David O., et. al.; Non-endoscopic biopsy techniques: a review; Expert Review of Gastroenterology & Hepatology; Volume 12, 2018 - Issue 2; https://www.tandfonline.com/doi/full/10.1080/17474124.2018.1412828
8. Stereotactic Brain Biopsy; 2020 American Association of Neurological Surgeons; https://www.aans.org/en/Patients/Neurosurgical-Conditions-and-Treatments/Stereotactic-Brain-Biopsy
9. Liquid Biopsy; NCI Dictionary of Cancer Terms; NIH National Cancer Institute; https://www.cancer.gov/publications/dictionaries/cancer-terms/def/liquid-biopsy
10 Liquid Biopsy; The American Association for Clinical Chemistry Lab Test Online; https://labtestsonline.org/tests/liquid-biopsy
11. Biopsies- Overview; RadiologyInfo.org; https://www.radiologyinfo.org/en/info.cfm?pg=biopgen#benefits-risks
12. What happens to biopsy and cytology specimens?; Cancer.org; American Cancer Society; https://www.cancer.org/treatment/understanding-your-diagnosis/tests/testing-biopsy-and-cytology-specimens-for-cancer/what-happens-to-specimens.html
13. Biopsy; Cancer.net; American Society of Clinical Oncology; https://www.cancer.net/navigating-cancer-care/diagnosing-cancer/tests-and-procedures/biopsy
14. Department of Health. Report of the review of NHS pathology services in England. London, DH. 2006. https://www.networks.nhs.uk/nhs-networks/peninsula-pathology-network/documents/CarterReviewPathologyReport.pdf
Leica Biosystems Knowledge Pathway content is subject to the Leica Biosystems website terms of use, available at: Legal Notice. The content, including webinars, training presentations and related materials is intended to provide general information regarding particular subjects of interest to health care professionals and is not intended to be, and should not be construed as, medical, regulatory or legal advice. The views and opinions expressed in any third-party content reflect the personal views and opinions of the speaker(s)/author(s) and do not necessarily represent or reflect the views or opinions of Leica Biosystems, its employees or agents. Any links contained in the content which provides access to third party resources or content is provided for convenience only.
For the use of any product, the applicable product documentation, including information guides, inserts and operation manuals should be consulted.
Copyright © 2026 Leica Biosystems division of Leica Microsystems, Inc. and its Leica Biosystems affiliates. All rights reserved. LEICA and the Leica Logo are registered trademarks of Leica Microsystems IR GmbH.